Project Description
BEYPRO2 – Clinical Trial
An evaluation of the efficacy beyond progression of vemurafenib combined with cobimetinib associated with local treatment compared to second-line treatment in patients with BRAFV600 mutation-positive metastatic melanoma in focal progression with first-line combined vemurafenib and cobimetinib
Nearly half of the patients with advanced melanoma harbor a valine to glutamine substitution (V600E) in codon 600 of the serine-threonine kinase BRAF (Davies et al 2002). Less common BRAF mutations such as lysine (V600K) or arginine substitutions (V600R) have also been reported (Eroglu et al 2016). In the past 5 years, two BRAF inhibitors that target these mutations, vemurafenib and dabrafenib, have been approved by the US Food and Drug Administration (FDA). These drugs have shown high rates of rapid response, with rates ranging from 48% to 59% in phase II and III trials (Chapman et al. 2011; Ascierto et al. 2013; Hauschild et al. 2012). Duration of responses is however limited in the majority of patients due to the development of acquired resistance, with median progression-free survival (PFS) in these patients ranging from 5.1 to 6.8 months (Sosman et al. 2012; Hauschild et al. 2012). Mechanisms of resistance to BRAF inhibitor therapy are diverse and include the reactivation of the mitogen-activated protein kinase (MAPK) pathway in over two-thirds of tumors, along with promotion of parallel signaling networks such as the PI3K–PTEN–AKT pathway (Shi et al. 2014; Rizos et al. 2014). Sequential therapy with a MEK inhibitor following progression on a BRAF inhibitor has not shown benefit, as no responses and a PFS of only 1.8 months was observed in a study of 40 patients, suggesting that resistance to BRAF inhibitors also confers resistance to MEK inhibitors (Kim et al. 2013). Therefore, the premise behind the subsequent clinical trials combining inhibitors of both MEK and mutant BRAF kinase was that they would help to delay resistance and result in higher rates and longer duration of responses and reduced toxicity respect to BRAF inhibitor monotherapy (Eroglu et al 2016). Patterns of progression with combined therapy are heterogeneous and progressive lesions often represent only a small amount of the total tumor burden. In this setting, a local treatment of progressing lesions can be provided without modifications of the ongoing systemic treatment. Even when a local treatment cannot be delivered, retrospective evidence in the BRAF monotherapy setting supports continuation of therapy in order to maintain partial inhibition of the pathway. The activity of treatment beyond progression with combination treatment has never been evaluated in a prospective trial.
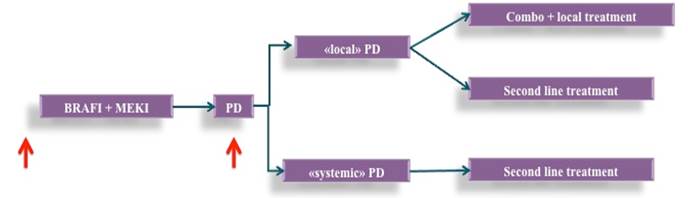
The aim of this trial is to evaluate the impact of combined cobimetinib and vemurafenib treatment beyond progression associated with local treatment of progressive lesions in terms of overall survival (OS) improvement in patients affected by metastatic melanoma with BRAFV600 mutation treated with vemurafenib in combination with cobimetinib who experienced focal progression. Patients with focal progression who are randomized to local treatment plus BRAF+MEK inhibitor treatment beyond progression will receive second line treatment with anti-PD-1 in case of systemic progressive disease. The switch to second-line treatment is only postponed until systemic progressive disease and all patients will ultimately receive a second line treatment with anti-PD-1. A translational study will be carried out in order to identify positive and negative biomarkers predictive of clinical outcomes in paired tumor DNA specimens from the same patients (tumor biopsies and peripheral blood), taken before therapy with BRAF+MEK inhibitors and after progression. This requires tumor biopsies at baseline and upon progression for all enrolled patients when feasible. As tumor tissue biomarkers, aberrations in main molecular pathways involved in melanoma pathogenesis will be measured through gene panels.
The primary objective of the study is to evaluate the efficacy (OS), of vemurafenib combined with cobimetinib associated with local treatment compared with second-line therapy, in patients with BRAFV600 mutation-positive metastatic melanoma in focal progression with first-line combined vemurafenib and cobimetinib.
Secondary objectives are to compare PFS of patients receiving treatment beyond focal progression vs second-line treatment; the adverse event profiles in patients receiving treatment beyond progression vs. second line treatment; to evaluate the prognostic role of focal versus non-focal progressive disease; to identify positive and negative biomarkers predictive of clinical outcomes useful to address each patient to a personalized therapy.
Partners:
Dr. Paola Queirolo, IRCCS AOU San Martino, IST, Genova (Study Coordinator); Prof. Giuseppe Palmieri, IRGB-CNR, Sassari (Translational Study Coordinator); Dott. Paolo Bruzzi, IRCCS AOU San Martino, IST, Genova (Design and Statistical analysis); Italy